Lung Disease
In the line of duty, fire fighters may experience occupational exposure to gases, chemicals, particulate and other substances with potentially damaging short and long-term effects on the respiratory system.
Previous studies performed during knock-down and overhaul phases show fire fighters may incur exposure to toxicants and respiratory tract irritants including: sulfur dioxide, hydrogen chloride, phosgene, nitrogen oxides, aldehydes and particulate. The combustion of building materials generates countless combustion products, with numerous new commercial compounds introduced annually.
Given the excessive exposure of fire fighters to respiratory irritants and toxicants, it is essential that firefighters recognize the importance of breathing apparatus use and take steps to minimize their risk of acute and chronic pulmonary disease.
Normal Lung Function
The normal human pulmonary system is made up of a number of components which work together to provide oxygen to the blood stream which is delivered to vital organs and remove waste products including CO2. The system includes the diaphragm, a muscle which through it’s downward movement increases the size of the pleural (lung) space, allowing inhalation. As the diaphragm relaxes, air is passively expired as shown in the picture below.
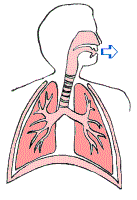
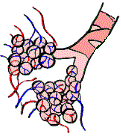
Inhaled air passes through the mouth and pharynx, travels down the trachea which divides into the right and left bronchi (upper airways), reaching the bronchioles and then the alveoli (distal airways). The alveoli are actually tiny air sacs which expand and contact like small balloons. Each alveolus has an arterial and venous blood supply, allowing “off-gassing” of waste gases including carbon dioxide – CO2 and “on-gassing” of oxygen – O2 necessary to sustain the body’s organs.
The solubility of irritant gases in water plays a role in determining penetration of the gases in the lung and effects of the irritant gas on the respiratory system. Water soluble gases are more likely to deposit in the upper or proximal airways (bronchi). Conversely, gases which are not water soluble are more likely to reach the distal airways resulting in damage to the lower airways (bronchioles and alveoli).
Acute Effects
The short-term effects of firefighting on the respiratory system have been studied on numerous occasions with varying results. These studies suggest that acute exposure to contaminants during firefighting:
1) May result in hypoxemia due to smoke inhalation.
2) May cause acute respiratory symptoms and acute decrements in lung function. Persistence of these decrements in some cases suggest decrements are not merely caused by irritant bronchoconstriction.
3) May cause acute increases in airway responsiveness.
These changes in lung function occur secondary to a variety of mechanisms, which may include reflex bronchoconstriction (constriction of the airways due to lung irritation) and smoke-induced airway hyperresponsiveness.
Long-Term Effects
It remains unclear whether or not the repeated exposure to smoke, which commonly occurs in firefighting, may be linked with chronic pulmonary disease. Several studies have been conducted looking at chronic respiratory related illness and deaths in firefighters. There are indications that repeated inhalations of smoke during routine firefighting activities can result in chronic bronchitis and abnormal lung function.
The results of many of these studies have not been clear cut, probably partly due to what is termed “the healthy worker effect”: firefighters, as a group, are healthier than the general population to whom they are compared. A result of the “healthy worker effect” is that fire fighters may appear to have reduced deaths and disease when compared to the general population, when in fact, the occurrence of disease in firefighters may be significantly higher. Additionally, only healthy fire fighters stay on the job. Those who become ill may leave the fire service without documented disability before retirement. Others may leave seemingly healthy, only to suffer the long-term effects long after their association with the fire service.
Prevention
There a number of steps that can be taken locally to reduce the rate of respiratory disorders.
a) An Effective Health and Safety Program – Declining lung function may be detected with periodic and baseline pulmonary function testing (PFTs). This testing allows documentation for treatment and future claims, and ammunition if corrective action needs to be taken. However, pulmonary function testing is only a record of damage which has already occurred. Preventing pulmonary damage is the key.
b) Training – It is important that every member of the fire service has an understanding of the respiratory risks of the fire environment, a goal which can only be accomplished through repeated training. People tend to follow rules and regulations more faithfully if they understand why they are adopted and how these procedures will conserve their health.
c) Use Respiratory Protective Equipment – Scientific studies show that SCBA equipment is effective in minimizing respiratory exposure to toxicants, carcinogens, gases and particulate during firefighting activity.
However, compliance may often be less than adequate. You can’t control what is generated by the fire, but you can control what you breathe. SCBA use is now universally accepted during the knock-down phase, but not during overhaul. Yet, during the overhaul phase many toxic constituents and particulates (such as asbestos) remain in the air, and a fire fighter’s risk of lung damage is still high. The IAFF strongly supports the use of SCBA’s during all phases of fire suppression.
d) Don’t Smoke – Smoking is strongly associated with chronic, irreversible, debilitating diseases including emphysema, heart disease and lung cancer. Encourage non-smokers not to start and those who smoke to quit. Smoking cessation programs are available through your local union representative and are endorsed by the IAFF. These cessation services are offered at a reduced rate and have been proven effective in helping those who want to quit achieve their goal.