
IAFF-IAFC Fire Service joint labor management wellness-fitness initiative
The International Association of Fire Fighters, in cooperation with the International Association of Fire Chiefs, committed to an unprecedented endeavor by collaborating with 10 of North America’s finest fire departments to build a stronger fire service by strengthening our foundation – the fire fighter.
A comprehensive wellness program that emphasizes physical, mental, and emotional well-being must be made available to recruits, active fire fighters, and retirees. The Fire Service Joint Labor Management Wellness-Fitness Initiative (WFI) has served as a guide for departments to engage in this pursuit for the past 25 years. Ultimately, any wellness-fitness program must be comprehensive, inclusive, accessible, and focused on behavioral change.
Leading the Way
Over the last 25 years, the IAFF has become the world’s leading authority on fire fighter health, wellness, and fitness. Through tireless efforts and a singular vision to improve the lives of fire fighters and their families, the IAFF has developed, implemented, supported, and advocated for numerous initiatives that directly target the most important issues affecting the health and well-being of members of the fire service. In this spirit, the IAFF continues to invest in strategic partnerships that will drive innovation in support of the physical, psychological and social well-being of every fire fighter.
The International Association of Fire Chiefs (IAFC) represents the leadership of fire fighters and emergency responders worldwide; its members are the world’s leading experts in firefighting, emergency medical services, terrorism response, hazardous materials spills, natural disasters, search and rescue, and public safety policy.
Partners on the Same Mission
Performance Redefined (PR) is a company that creates short- and long-term education, coaching, and exercise solutions to address the health, fitness, and performance needs of fire fighters. As a technical advisor to the IAFF and IAFC for many years, PR has amassed extensive experience working directly with fire fighters and is committed to the mission of improving wellness and fitness in the fire service. PR is honored to support the IAFF and IAFC in the ongoing development and implementation of the WFI.
Building on a Strong History

In 1997, the IAFF and IAFC launched the Wellness-Fitness Initiative (WFI) and committed to leading an innovative charge to improve the health and wellness of all uniformed fire department personnel. Since its inception, the WFI has become the principal most comprehensive resource in support of fire fighter wellness and fitness, largely because of the efforts made by the union leaders, fire chiefs, subject matter experts, and local champions from the 10 task force cities (FDNY, Fairfax County, Calgary, Seattle, Indianapolis, Phoenix, LA County, Austin, Miami-Dade, and Charlotte) who have worked collaboratively to identify best practices. But there is also recognition that updates are needed to address the evolving demands of the profession and emerging trends in health, wellness, and fitness research.
In addition to highlighting what is important, we must prioritize the implementation process (i.e., how to make things work) so that departments are provided with the necessary support to improve the health and well-being of their members. Central to this mission are guidelines to define, pursue, support, restore, and promote wellness and strategies to target the specific behaviors (e.g., exercise, diet, sleep) known to influence fire fighter health, fitness, and overall well-being.
An Expanded Task Force
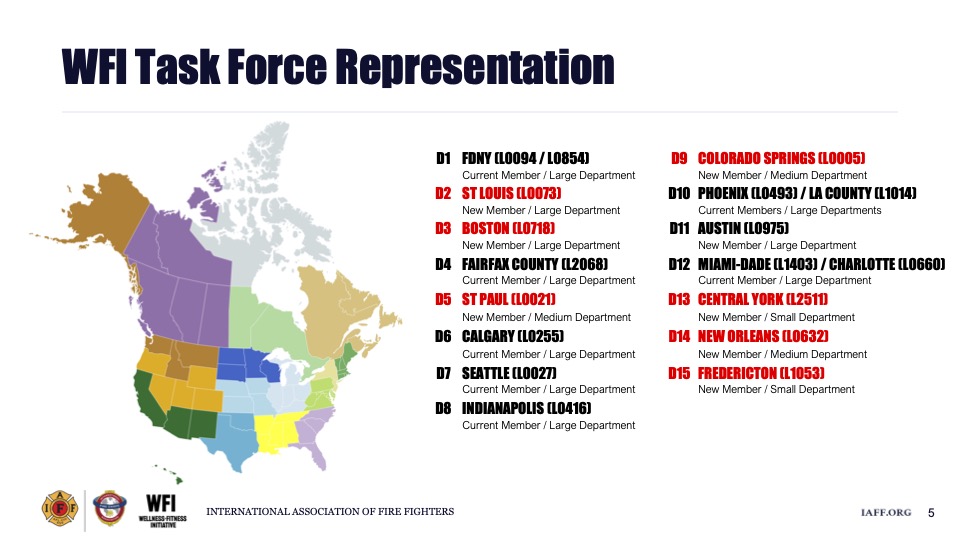
In support of future WFI initiatives, and to ensure the WFI Task Force reflects the composition of the fire service at large, the IAFF and IAFC made the decision to expand the WFI Task Force to include at least one department from IAFF Districts 1 through 15 and all 8 IAFC Divisions. The Task Force also includes representation from large (600+ members), medium (200+ members), and small (<200 members) departments to ensure diversity in perspectives. Each fire chief and Local president have certified their commitment by pledging to:
- Serve as a district representative and model for other departments to learn from.
- Share resources, data, and implementation processes in support of the broader fire service community.
- Engage with and support the WFI Task Force via formal networks created and fostered by the IAFF and IAFC.
- Participate in WFI Task Force initiatives led by the IAFF and IAFC in support of fire fighter wellness and fitness.

Igniting Change
The IAFF was recently awarded a FEMA grant to restructure and refocus the WFI to better serve the unique wellness-fitness needs of the fire and EMS by placing a larger focus on best practice guidelines and program implementation. This new resource will be branded as, “The IAFF/IAFC Wellness-Fitness Initiative – Igniting Change,” to better reflect the aims and scope of the revision, and it will be structured in such a way that any department regardless of constraints or circumstances can use the WFI to outline a path for themselves to follow. The WFI will be organized as a repository of evidence, a collection of best practice guidelines, and an actionable implementation roadmap that compliments federal and local standards using the newly established wellness-fitness framework (see below).
The FEMA grant project includes six phases, each with specific objectives and desired outcomes, and will be overseen by the IAFF, IAFC, and PR. A group of uniformed and non-uniformed subject matter experts (SMEs) with relevant expertise and experience is currently supporting the project by reviewing and drafting materials. A brief description of each phase of the project is outlined below.
Phase 1
Review the 4th edition of the WFI to identify gaps and opportunities, and to “map” the aims, objectives, and content to the newly established wellness-fitness framework.

Phase 2
Assemble working groups comprising SMEs from Task Force city departments and the broader community to discuss priorities, review material, and develop content. Each working group meets independently and collectively with the entire Task Force every month.
Phase 3
Meet with stakeholders from each Task Force city department to discuss prior and current wellness-fitness activities, outcomes, obstacles, perspectives, lessons learned, etc. These meetings will be used to create implementation case examples for the revised WFI.
Phase 4
Consolidate information gathered from stakeholder meetings in Phase 3. Specifically, the tools, strategies, and tactics used to assess personal and organizational needs; change, reinforce, and restore target behaviors; and evaluate program processes and outcomes will be summarized and consolidated into “Best in practice” recommendations and “how-to” guidelines.
Phase 5
Produce a first draft of the resource, including all supplementary materials, case examples, and supporting evidence.
Phase 6
Fire chiefs, union executives, and subject matter experts from each Task Force city department, IAFF and IAFC staff, and a group of independent reviewers will be asked to provide feedback regarding the scope, accessibility, inclusivity, usability, and appeal of the WFI – Igniting Change resource.
Project Updates
Related programs
Candidate Physical Ability Test (CPAT)
Fit to Thrive (F2T)
WFI-Igniting Change
On October 28-29, 2024, 58 subject matter experts (SMEs) met in Washington, DC to discuss the WFI. This group included representatives from each of the 17 WFI Task Force Cities, staff from the IAFF, IAFC and Performance Redefined, and advisors from multiple fields of work assisting fire fighters (i.e., physicians, academics, fire chiefs, labor executives). The overall aim of the meeting was to discuss the aims, impact, and structure of the WFI to better direct the on-going efforts of the Task Force and the working groups that have been assembled to support the revising of the WFI.
Please click here for a brief summary of the discussion points and meeting outcomes.
About the WFI
The original aims of the WFI include:
- Overcome the historic fire service punitive mentality of physical fitness and wellness issues
- Move beyond negative timed, task-based performance testing to progressive wellness improvement
- Require a commitment by labor and management to a positive individualized fitness/wellness program
- Develop a holistic wellness approach that includes medical, fitness, rehabilitation, and behavioral health
Fire fighters must continue to respond to emergency incidents that require extreme physical output and often result in challenging physiological and psychological outcomes. Such situations, over time, can and do affect the overall wellness of the fire fighting and emergency response system. Tomorrow’s fire service requires that we keep our fire fighters fit today. The ultimate goal of the Fire Service Joint Labor Management Wellness-Fitness Initiative is to improve the quality of life for all fire fighters.
The participating departments on the Task Force are: Austin, TX Local 975; Calgary, AB Local 255; Charlotte, NC Local 660; Fairfax, VA Local 2068; Indianapolis, IN Local 416; Los Angeles County, CA Local 1014; Metro Dade, FL Local 1403; New York City, NY Local 94 and Local 854; Phoenix, AZ Local 493, and Seattle, WA Local 27.
This system proves the value of investing wellness resources over time to maintain a fit, healthy, and capable fire fighter throughout his/her 25-30+ year career and beyond. An effective program should realize significant cost savings in lost work time, workers’ compensation, and disability.
The Mission
An overall wellness/fitness system must be developed to maintain fire fighters’ physical and mental capabilities and should be the objective of every fire department in cooperation with its local IAFF affiliate. While such a program may be mandatory, the agreement to initiate it must be mutual between the administration and its members represented by the local union. Any program of physical fitness must be positive and not punitive in design; require mandatory participation by all uniformed personnel in the department once implemented; allow for age, gender, and position in the department; allow for on-duty-time participation utilizing facilities provided or arranged by the department; provide for rehabilitation and support for those in need; contain training and education components; and be reasonable and equitable to all participants.
The program must address the following key points:
- Confidential behavioral, medical, and fitness evaluations
- Development of a physical fitness and wellness program that is educational and rehabilitative and not punitive
- Requires a commitment by labor and management to a positive individualized fitness/wellness program
- Development of a holistic wellness approach that includes: Fitness, Medical, Rehabilitation, and Behavioral health
Candidate Physical Ability Test
The Candidate Physical Ability Test (CPAT) was developed as a fair and valid evaluation tool to assist in selecting fire fighters and ensure that all fire fighter candidates possess the physical ability to complete critical tasks effectively and safely. The CPAT program covers every aspect of administering the CPAT, including recruiting and mentoring programs, providing recruits with fitness guidance to help prepare them for the CPAT, and setting up and administering the test. The entire validation process and the legal issues that departments might face when implementing the actual program are discussed in detail.
Fit To Thrive
We are leading an innovative charge to improve fire fighter health and wellness by launching the FIT TO THRIVE (F2T) program. Born as an extension of the IAFF/IAFC Peer Fitness Trainer (PFT) program, F2T is designed to support the WFI by helping more fire fighters be more active, more often so they can experience the benefits of regular exercise. It is comprehensive, inclusive, accessible, and focused on behavior change.
The IAFF/IAFC Task Force has determined that successfully implementing the Wellness-Fitness Initiative and the CPAT requires a fire fighter in each department who can take the lead. This individual must be able to design and implement fitness programs, improve the wellness and fitness of their department, and assist with the physical training of recruits. This need for a department-level leader led to the development of Fit To Thrive (F2T).